 (See "Anticoagulation for prosthetic heart valves: Management of bleeding and invasive procedures", section on 'Management of bleeding'.) For such patients, we anticoagulate with heparin during the acute setting whenever possible because it is typically quicker to reverse in the event of hematoma expansion. In addition, for most patients with acute SDH who are managed nonoperatively, we reverse anticoagulation to reduce the risk of SDH enlargement.īy contrast, for some patients with a chronic or small acute SDH and no signs of increased ICP who are receiving anticoagulation for a compelling indication such as a mechanical heart valve, the risk-benefit calculation may favor continued anticoagulation with close observation of neurologic status. Reversal of anticoagulation is required for patients with acute or chronic SDH prior to surgical intervention. We balance the hemorrhagic risks of anticoagulation with the thrombotic risks of reversal at an individual level. Reversing anticoagulation - For most patients with SDH who are taking anticoagulants, we discontinue these medications and give agents to reverse anticoagulant effects. The clinical assessment typically includes the Glasgow Coma Scale ( table 2), a simple clinical scale to quantify deficits for patients with brain injury. (See "Initial management of trauma in adults", section on 'Primary evaluation and management'.)Ī neurologic examination is performed to determine the severity of initial neurologic deficits and provide a baseline to assess subsequent deterioration. The initial evaluation of adult patients with trauma is discussed in greater detail separately. Patients with SDH associated with trauma should also undergo a structured primary survey to identify and prioritize management of other injuries. Initial assessment and emergency management - The initial assessment of SDH includes airway management for patients with drowsiness or severe bulbar symptoms. Patients with acute or chronic SDH require urgent initial assessment of clinical status to determine the need for surgery and the medical interventions needed to mitigate adverse outcomes ( algorithm 1). INITIAL MANAGEMENT - SDH can be a neurologic emergency that may cause irreversible brain injury and death caused by hematoma expansion, elevated intracranial pressure (ICP), or brain herniation. (See "Traumatic brain injury: Epidemiology, classification, and pathophysiology".).(See "Spontaneous intracerebral hemorrhage: Pathogenesis, clinical features, and diagnosis".).(See "Perimesencephalic nonaneurysmal subarachnoid hemorrhage".).(See "Nonaneurysmal subarachnoid hemorrhage".).(See "Aneurysmal subarachnoid hemorrhage: Epidemiology, risk factors, and pathogenesis".).(See "Intracranial epidural hematoma in adults".).Other forms of intracranial hemorrhage are discussed elsewhere. (See "Intracranial subdural hematoma in children: Clinical features, evaluation, and management".). 
(See "Intracranial subdural hematoma in children: Epidemiology, anatomy, and pathophysiology".).(See "Subdural hematoma in adults: Etiology, clinical features, and diagnosis".).Other aspects of SDH are reviewed separately.  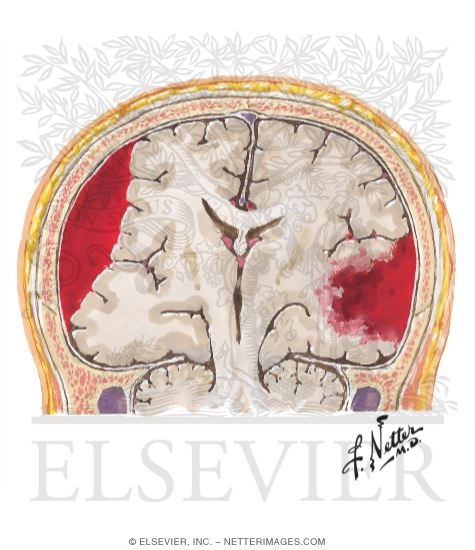
A rapid overview summarizes the clinical features, evaluation, and management of SDH in adults ( table 1). The management and prognosis of SDH will be discussed here. INTRODUCTION - Subdural hematoma (SDH) is a form of intracranial hemorrhage characterized by bleeding into the space between the dural and arachnoid membranes surrounding the brain. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
